There are scores of people out there who are allergic to penicillin.
Or are they?
“I see so many patients who say, ‘My mom told me I was allergic to it,’ or something along those lines, and it’s this label they carry with them into adulthood,” said MUSC Health allergist Emily Campbell, M.D.
But for the vast majority of those people, Campbell said, that’s just not the case anymore. And, in some instances, they never really were.
“About 10% of kids who are prescribed amoxicillin for an ear infection, or something like that, will get a rash,” she said. “Day 3, 4, 5 – it’ll pop up, typically as some blotches on the trunk. It lasts a few days and then goes away. Generally speaking, that is not a true allergy, rather just a side effect of the antibiotic.”
This is important for many reasons; those unable to take penicillin and its family of related drugs safely have been found to have a higher rate of surgical site infections, longer hospital stays and higher health care costs, just to name a few. But possibly where this creates the biggest issue is when a woman becomes pregnant.
According to Campbell, about 1 in 3 women test positive for group B strep, a bacteria that lives in the vaginal canal. Though perfectly harmless to the carrier, it can wreak havoc on a baby and its brand-new immune system. If an expectant mother has – or believes she has – an allergy to penicillin, this takes away one of the doctor’s greatest weapons given during the birthing process, ampicillin, an antibiotic known to protect babies from contracting it as well as reducing the subsequent hospital stay of mom and child.
The past two decades or so have been a boon of discovery for immunologists on this front, leading to a number of studies. One such study was conducted by Campbell herself along with College of Medicine chief resident for internal medicine, Rosemary Moak, M.D.; fellow allergists Kelli Williams, M.D.; and Maria Streck, M.D.; OB-GYN Gwen Lazenby, M.D.; fourth-year medical student Caroline Nassab; and Grace Weatherford, R.N. Over the course of a year, the trio looked at more than 200 pregnant patients who believed they were allergic to penicillin, and in the end, they found that more than 90% of them weren’t.
“Yeah. Pretty cool. That’s a big win right there,” Campbell said.
In fact, Campbell cited another study that followed patients who had anaphylaxis – a severe, life-threatening allergic reaction that can lead to death – over the course of 10 years. By the end of that time frame, 80% of those people no longer had an adverse reaction to the drug.
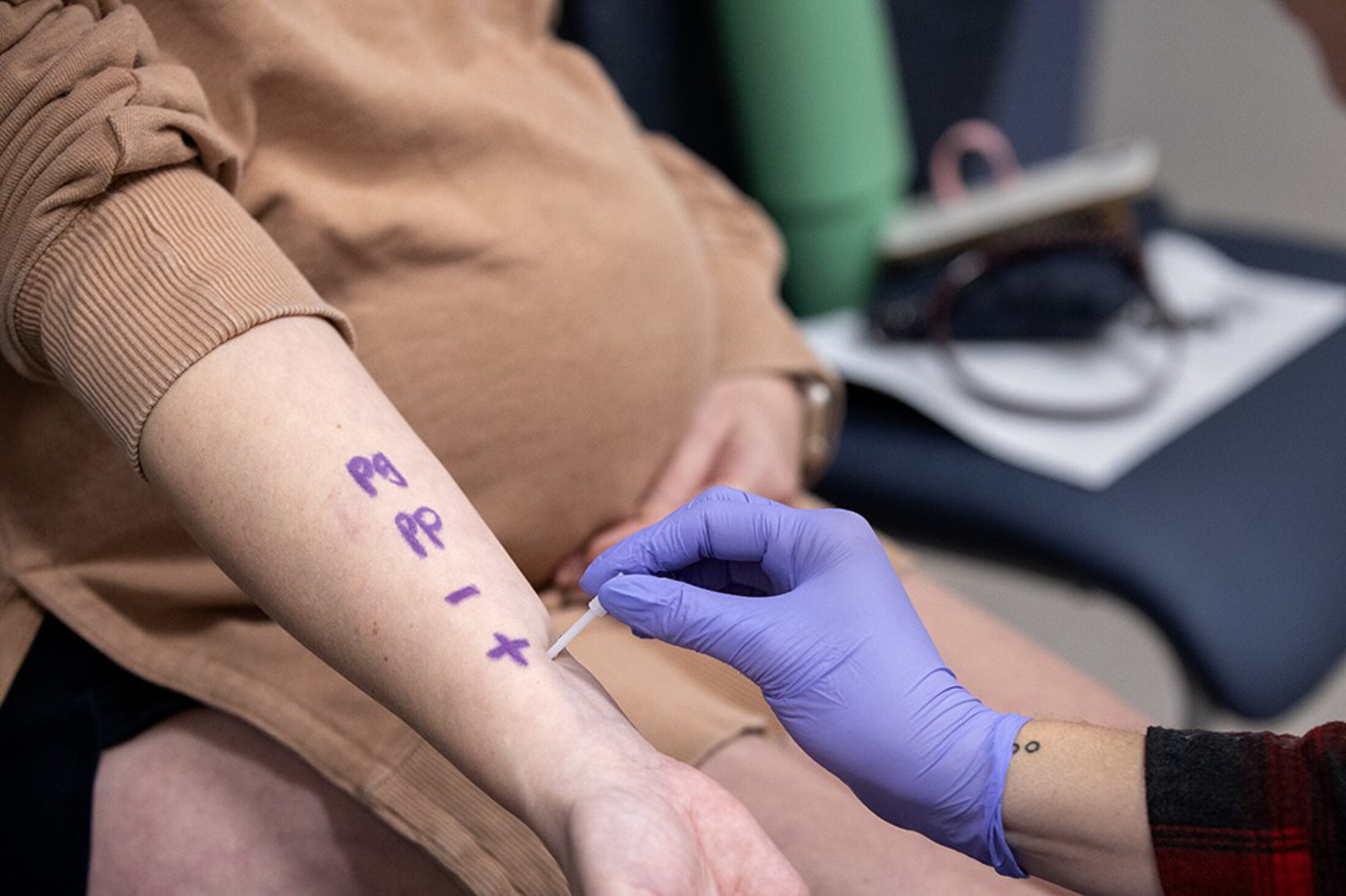
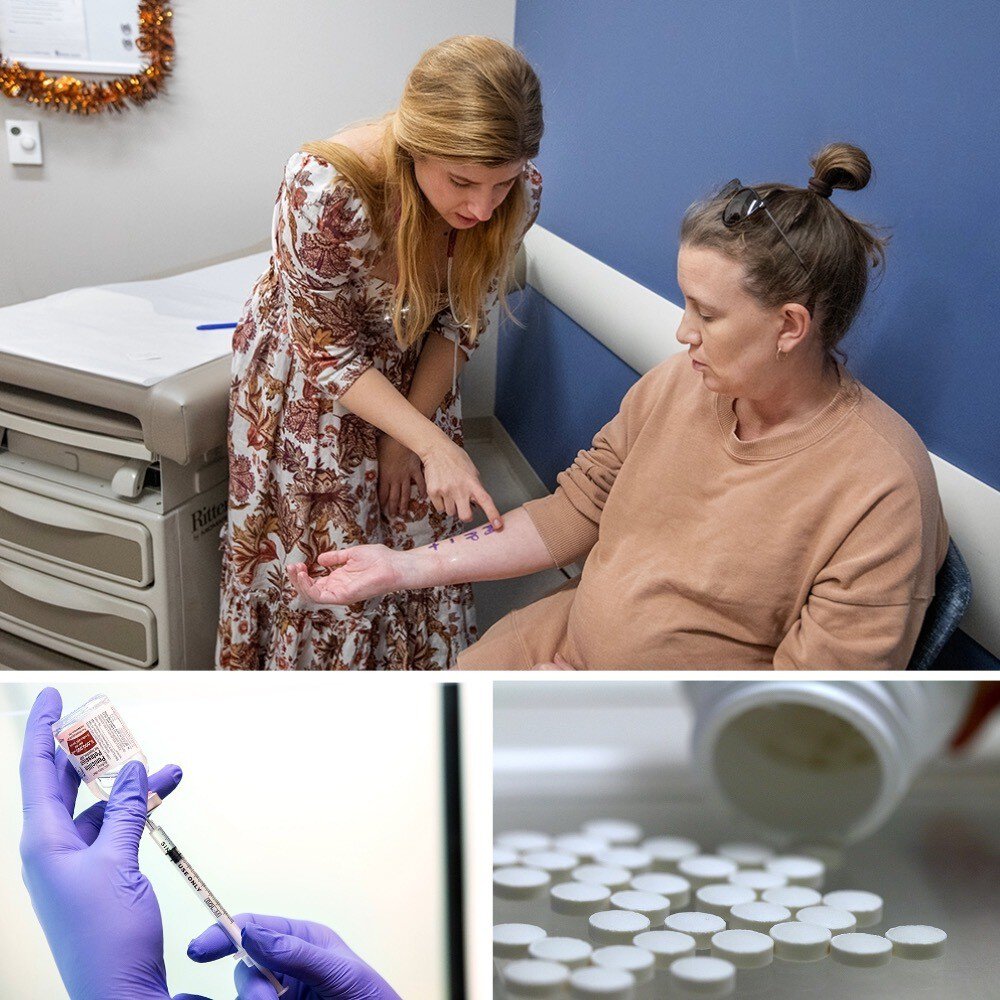
Today, Campbell said she tests as many as two to three patients a week for penicillin allergies. That process, she explained, is a relatively quick, FDA-approved, three-step process, all of which happens in the doctor’s office.
Step 1, they put a little of the drug on the skin, then wait 15 minutes. If the patient doesn’t have a reaction, it’s on to Step 2, intradermal testing, where they use a needle to put a small, dilute amount of the drug underneath the surface of the skin. Again, the patient waits 15 minutes. If given the thumbs-up, it’s on to Step 3, orally taking the medicine. If, after 45 minutes, the patient is showing no signs of distress, they are generally in the clear (the test is 94% predictive), forever dropping the label of “allergic to penicillin.”
Campbell even said if a patient knows her medical history and clearly recalls only having had a mild rash in conjunction with the drug, they can often skip right to Step 3, shaving a half-hour off the process.
“It really is a breeze,” she said. “And if it turns out they aren’t actually allergic, it’s so incredibly valuable, for us as providers, to have that family of antibiotics at our disposal during delivery.”
Recent Patient Journeys stories





